Retinoblastoma
Retinoblastoma clinical presentation
The symptoms of the disease at diagnosis are variable, depending upon the stage of the disease and how the eyes are affected. The two most common signs of RB are leukocoria (white pupil), which is seen in approximately 60% of patients, and strabismus (misaligned eyes) in 20% of them5 4. When the disease is more advanced, patients present with their eye/s protruding out of the orbit (proptosis) and the eye/s enlarged. Patients might also present with glaucoma, which is caused by increased intraocular pressure. The main symptoms of glaucoma are pain, vision loss and optic nerve changes seen on a fundoscopic examination.
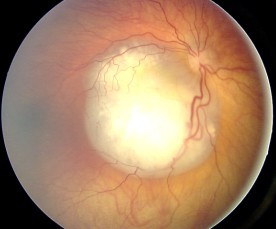
When the disease advances, it usually spreads to the orbit, brain and and/or the bone marrow. Unfortunately, prognosis of patients with brain and bone marrow disease is poor, and chances of cure are dismal.
Trilateral RB is a syndrome that occurs in 3-5% of patients with bilateral RB and consists of hereditary/bilateral RB associated with an intracranial neuroblastic tumour. These brain tumours belong to the family of primitive neuroectodermal tumours (PNET) and are generally located in the pineal region of the brain. However, 20 to 25% of them occur in the suprasellar and parasellar region3. These tumours generally present more than 20 months after the diagnosis of bilateral RB, and usually affect the second or third generation of bilateral RB patients7. Prognosis is poor for patients with trilateral RB, with a cumulative 5-year survival rate of 27% if diagnosis is done by screening and the tumour is small in size7. These patients need very intensive treatment and only a proportion of them survive.
Of note, approximately 8% of patients with bilateral RB develop pineal cysts3, not to be confused with the brain tumours associated with trilateral RB. These benign lesions require no intervention unless they are symptomatic. Most pineal cysts remain the same size or resolve over the course of years8.